Stem Cell Therapy for Parkinson's Disease Latest Potential Safe & Effective Treatment for Parkinson’s Disease
What causes Parkinson’s disease?
Parkinson’s disease (PD) is a neurodegenerative condition that causes progressive loss of motor function and impaired balance. A part of the brain called the substantia nigra contains neurons that produce dopamine. In PD, the loss of these neurons leads to declining dopamine and neuronal connections over time. These changes cause the many debilitating and life-altering symptoms of PD.
Common symptoms of Parkinson’s disease include:
- Tremor/shaking of the extremities
- Slowness of movement
- Shuffling gait
- Muscle stiffness
- Expressionless face
- Painful muscle cramps
PD is caused by a combination of environmental and genetic influences and there is currently no known cure. Neuron loss is usually slowly progressive and symptoms don’t typically show up until ~50% of the dopamine-producing neurons have been lost1. Diagnosis is made clinically based on history, signs and symptoms, and physical exam.
The Scientific Rationale Behind Stem Cell Therapy for Parkinson’s Disease
Currently, there is no known cure for Parkinson’s disease. The standard-of-care treatments do not restore lost dopamine neurons. Most drugs for Parkinson’s disease also have severe side effects that tend to lower the quality of life. They also do not slow down the progression of the disease. This is where stem cell therapy can uniquely deliver benefits.
Stem cells are immature (also called “undifferentiated) cells that can turn into a number of other cell types. They can also expand in numbers into more of the same stem cells. For example, a mesenchymal stem cell can develop into a fat cell, neuron, cartilage, and many others. In stem cell therapy, these stem cells are placed in the area of need, where they can then replace degenerated tissues.
You may have heard of stem cell therapy being used for degenerated cartilage, like in joints. However, many other degenerative conditions can benefit from stem cell therapy, such as neurodegenerative diseases like Parkinson’s disease.
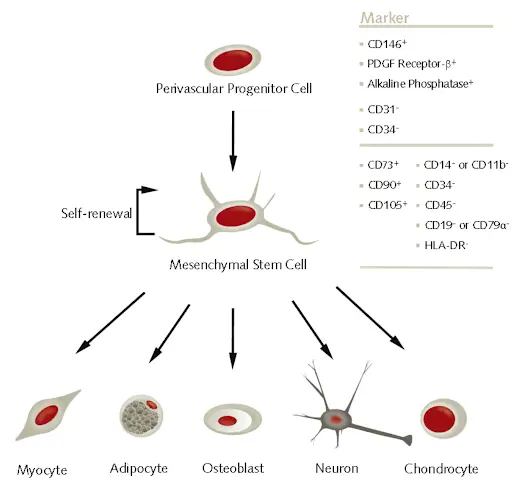
There are two types of stem cells: embryonic and adult stem cells. Embryonic stem cells come from embryos, whereas adult stem cells come from adult tissues.
At Nashville Regenerative, we use only adult stem cells harvested from the patient’s body to treat the patient. This minimizes the risk of tissue rejection and eliminates any need for immunosuppressive drugs, unlike in other types of transplants.
Adult stem cells exist throughout your body. However, different kinds of stem cells exist in different places. Mesenchymal stem cells are commonly used in stem cell therapy because they are easy to harvest and can develop into many important cell types.
Mesenchymal stem cells have been isolated from the following locations in the human body:
- Bone marrow
- Adipose (fat) tissue
- Periosteum (outside layer of bone)
- Tendon
- Lung
- Umbilical cord
Bone marrow and fat tissues are common sites for stem cell harvesting. After harvesting, the stem cells can be isolated from your other tissues and used immediately, or they can be cultured in 6 - 8 weeks. When stem cells are cultured, they are grown in a nutrient medium, where they expand in numbers. This increased stem cell dose can then be injected, increasing the likelihood of beneficial results
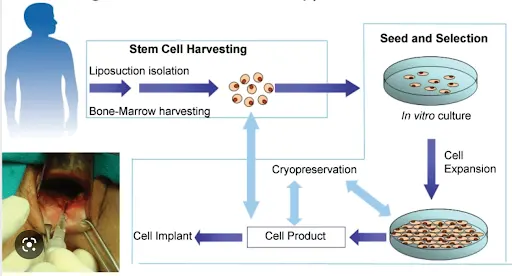
Parkinson’s disease (PD) is a neurodegenerative disease, thus a cell regenerative approach may provide benefits. Mesenchymal stem cells can further develop into neurons to replace some of the lost brain cells and dopamine in Parkinson’s disease.
Once harvested, the stem cell suspension is injected into the bloodstream and into the nervous system through the spine, where the stem cells can then enter the brain and seed in the area of neuron loss.
For patients who need higher doses of stem cells, we culture their stem cells in the lab to expand the number of these stem cells. Our US-based stem cell lab facility is FDA-registered, ISO-7 certified and certified in Good Manufacturing Practices. They will then schedule a procedure to receive the stem cell treatment once the cultures are ready.
One benefit of mesenchymal stem cells is that they home in on sites of inflammation and injury 3. The neuron damage in PD may actually attract the stem cells to go to the right place.
By increasing the number of neurons in the brain area of degeneration in PD, there is more dopamine production and neuron function available. This alleviates symptoms from more of the root of the issue, versus trying to increase dopamine with medications alone.
Stem cell therapy for Parkinson’s disease is a helpful adjunct to other treatments you may be doing currently.
- Harvest stem cells from your bone and/or fat
- Inject some stem cells right away
- Culture some stem cells in our lab to increase cell numbers
- Get the stem cells back and inject the concentrated suspension (~6 - 8 weeks later)
The effects of stem cell therapy can be highly individual. Many factors determine the efficacy of stem cell therapy for Parkinson’s disease, including disease stage and what you’re hoping to see improve. However, in our experience, 70-80% of people will experience some level of symptom improvement.
Clinical trials have been underway since the 1980s, demonstrating various levels of efficacy and generally fewer side effects than standard-of-care treatments. Because stem cells become new neurons that replace the destroyed ones, the benefits may continue for several years. Beyond the ability of mesenchymal stem cells to differentiate into neurons, they also send cell signals to other cells. This is how the transplanted stem cells help counteract the inflammation and excess immune response that contributes to the disease process.
Early studies of stem cells in PD were done in animals, with stem cells being placed directly into the brain. These studies largely demonstrated improvement in PD symptoms and protection from neuron loss. Interestingly, these animal studies show that stem cells may exert neuroprotective effects by modulating the immune system, even if the stem cells never develop into dopamine-producing neurons. Similar studies have since been followed up in humans.
In a 2016 human study, 21 adults with PD underwent 2 separate stem cell implants into the striatum region of their brains. Some underwent both procedures within a year, others within 1-3 years, and the rest at some time after the 3-year mark. After the first stem cell implant, the patients had significant improvement in PD symptoms based on the four different standardized PD questionnaires. Furthermore, these improvements lasted up to 57 months. Symptoms that improved included the areas of motor function, cognition/behavior, and activities of daily living.
In an important 2017 study, stem cells were implanted into the brains of monkeys used as PD models. Regardless of whether the stem cells came from PD donors or those without PD, the stem cells led to new neuron formation and the monkeys had recovery in functional symptoms of PD. This demonstrates that even though someone has PD, their own stem cells can provide benefits.
In a 2019 clinical study of 8 patients, stem cell therapy resulted in a noticeable improvement in motor and neurologic functions in 7 of the 8 patients. These patients then underwent an annual evaluation each year for 4 years. PD symptoms were slightly less improved at the 4-year mark, but still better than the baseline of 4 years prior 5.
While the majority of research has been in animals, the potential of stem cell-based therapies based on these studies is clear and extremely promising. This is further supported by some of the first human studies showing benefits. This also matches our clinical experience. Importantly, these therapies have shown safety and minimal need for immunosuppressive therapies to avoid cell rejection.
Given that the effects of stem cell transplants can be highly individual, we mainly use a non-surgical stem cell transplant to deliver stem cells into your nervous system. This makes it possible for our patients to reap the benefits of stem cell therapy without the risk and recovery time of surgery.
Also promising, the benefits of stem cell therapy may be increased by other lifestyle factors such as exercise, physical therapy, and nutrition.
There is currently no known stage of Parkinson’s disease that stem cell therapy works best for. Since it acts regeneratively, it may help at any stage. Typically, the earlier you treat any health condition, the better results you can expect.
However, as the disease progresses, even small positive changes can make a world of difference. Generating new neuron connections in late-stage Parkinson’s disease may significantly improve symptoms and quality of life.
The cost depends on the specific treatment you will be undergoing and how many treatment sessions you need. Book a consultation with us today to get your personalized stem cell therapy treatment plan.
Typically, you will need 1 - 2 treatments, depending on the plan of care established between you and your doctor. All treatment appointments are in person, but the initial consultation and follow-up can be done by phone.
Some people do come back for additional treatments over the course of months or years. This largely depends on the stage of your disease, how well you respond to the treatment, and what your treatment goals are.
Your patient journey with stem cell therapy for Parkinson’s disease
Step 1: Application and initial consultation
Our questionnaire and initial consultation help us determine whether you’re a good candidate for stem cell therapy, along with the best treatment plans for you. Our patient advocate will walk you through the process, pricing, and payment plans.
Step 2: Physical exam
You’ll come in for a physical exam in preparation for the treatment and also to assess your current symptoms and health status.
Step 3: Stem cell collection
Your procedure will begin where we harvest cells from your bone marrow or fat tissues. We will then isolate the stem cells from these tissues in the clinic before administering your first treatment.
Step 4: Stem cell culture
If applicable, we will send your stem cells to the lab to expand them in numbers.
Step 5: Future treatments
Your future stem cell treatments will be done using your cultured stem cells.
Step 6: Follow-up appointments
Our team will keep in contact with you to monitor your treatment progress and support you through your recovery.
Advantages of Stem Cell Therapy vs Standard Treatments and Other Alternative Treatments
Current standard-of-care treatments for Parkinson’s Disease and their shortfalls
No treatment is known to either cure or slow the progression of Parkinson’s disease 12. Since there is no known cure, treatments are aimed at symptom improvement and management. These treatments have different results based on the level of disease progression and individual characteristics of drug response. Many of the current medication treatments come with significant side effects which may require other drugs to try and manage, and they may make the quality of life just as bad as the disease.
This typically includes a combination of hands-on bodywork and movement therapy. Physical therapy may be beneficial in relieving muscle tension and supporting walking and other movement difficulties. In these ways, physical therapy can significantly help improve quality of life.
Physical therapy, however, will not do anything to slow disease progression, so it may become less and less effective over time as the disease worsens.
This focuses on tasks of daily living that may be difficult, such as cooking or getting dressed. An occupational therapist will help you with solutions for these tasks and help ensure an environment that is safe from things like trip hazards.
Difficulty swallowing (dysphagia) and trouble speaking are common among Parkinson’s patients. Speech and language therapy is like physical therapy for these specific areas of great importance.
These two medications are the mainstay of conventional Parkinson’s disease treatment.
Levodopa is a precursor to dopamine. By providing your brain with levodopa, it can then convert it to dopamine, which is depleted in PD.
Carbidopa is commonly administered along with levodopa. Carbidopa inhibits levodopa from being converted to dopamine in other areas of your body outside of your brain (periphery). In this way, carbidopa supports more levodopa to dopamine conversion in your brain where it’s needed.
While this therapy can improve some Parkinson’s symptoms, it does not slow progression and there are common side effects that could prove to be just as bad as Parkinson’s. At some point, the neuron loss becomes more than levodopa/carbidopa can compensate for. Increasing doses become less effective and intolerable as they come with more side effects.
Potential side effects of levodopa/carbidopa therapy include:
- Dyskinesia (involuntary, erratic, sometimes writhing movements) – This occurs in up to 80% of people taking levodopa for 3 years. Other involuntary movements include abnormal mouth movements and bobbing of the head.
- Akinesia – This is an absence of movement or potentially slow movements (bradykinesia) that come in on/off episodes.
- Dizziness
- Drowsiness
- Headache
- Insomnia
- Depression or mood changes
- Nausea & vomiting
- Memory impairment
- Nightmares
- Sudden onset sleepiness
- Peripheral neuropathy
- Psychosis
Many other potential side effects of levodopa and carbidopa exist. Once present, the dyskinesia symptoms may continue even if the dose is reduced.
These medications bind to the same receptors as dopamine and stimulate its function. They are not as strong as levodopa but sometimes can help decrease the dose of levodopa.
Possible side effects include:
- Same as levodopa
- Leg swelling
- Feeling generally ill
- Sleepiness
- Dizziness
Monoamine oxidase-B (MAO-B) is an enzyme in the brain that breaks down dopamine. A number of medications exist that block this enzyme. The result is less dopamine breakdown, therefore prolonging dopamine levels in neurons.
Possible side effects of MAO-B inhibitors include:
- Nausea
- Dry mouth
- Lightheadedness
- Constipation
- Confusion
- Hallucinations
Animal evidence has suggested that this class of medications may slow Parkinson’s disease progression, but this has not been proven in human trials
This is an antiviral medication that also has some brain effects that act in a calming way to the nervous system. It is commonly used to treat dyskinesia side effects of levodopa.
- Side effects include:
- Confusion
- Hallucinations
- Leg edema
- Rash
Catechol-O-methyltransferase (COMT) is an enzyme that breaks down levodopa. COMT inhibitors block this enzyme, increasing levodopa levels. These medications are typically used in late-stage Parkinson’s disease.
Side effects include:
- Feeling generally ill
- Diarrhea
- Abdominal pain
Acetylcholine is the primary neurotransmitter in the brain and entire body. Anticholinergics block acetylcholine receptors, and can help with tremor and cramping. They do not typically help with other symptoms of Parkinson’s disease.
Side effects include:
- Dry eyes
- Dry mouth
- Urinary retention
- Confusion
Deep brain stimulation involves a small device implanted under the skin, similar to a pacemaker. The device has wires run to specific parts of the brain to stimulate the neurons with electrical impulses.
This again is not curative but may improve symptoms. Similarly to levodopa, as the disease progresses, the treatment loses effectiveness.
Why Nashville Integrative Therapy?
We are passionate about delivering safe and effective treatments to our patients, especially when standard-of-care treatments fall short. Over the years, we’ve seen the immense life-changing benefits of stem cell therapy first-hand and we’re passionate about making it available to you.

About Dr. Ethan Kellum, MD
Dr. Ethan Kellum is a pioneer in interventional and regenerative orthopedics. As a sports medicine specialist who is fellowship-trained in orthopedic surgery, Dr. Kellum is an expert in musculoskeletal injuries and joint conditions. Although he still performs shoulder and knee surgeries, his main focus has become regenerative medicine, especially stem cell therapy, to keep patients out of the operating room.
Dr. Kellum is a native of Henderson, Tennessee and attended Jackson Christian School and Freed-Hardeman University. He earned a medical degree from the University of Tennessee Health Science Center College of Medicine in Memphis. After a residency in orthopedic surgery at the Medical College of Georgia, he then completed a surgical fellowship in sports medicine, shoulder, and advanced arthroscopy at the renowned New England Baptist Hospital and Boston Children’s Hospital in Boston, Massachusetts. During his fellowship, he served as assistant team physician for the NBA’s Boston Celtics, and for both Harvard and Tufts University athletics. Dr. Kellum is a member of the prestigious Alpha Omega Alpha Medical Honor Society. Dr. Kellum has been actively involved in orthopedic surgery research throughout his medical career. He also has authored and co-authored several peer-reviewed orthopedic surgery articles and book chapters.
Beyond his credentials, Dr. Kellum is a compassionate, committed surgeon who has care and love for each and every patient he sees. It is Dr. Kellum’s passion to create an environment that treats and cares for the whole patient- mind, body and soul holistically. He aspires to build the full-body health and longevity of each of his patients through regenerative orthopedics, nutrition, exercise and complementary medicine. Dr. Kellum works to create an innovative and patient-centered atmosphere that feels like home.
What our patients are saying about our stem cell therapy
Got questions?
Speak to our patient advocate
Frequently Asked Questions
The FDA has not currently approved the majority of stem cell therapies in the U.S., despite demonstrated research of safety and efficacy. “Currently, the only stem cell treatments approved by the Food and Drug Administration (FDA) are products that treat certain cancers, and disorders of the blood and immune system.”
Stem cell therapy is currently not covered by insurance. As more research is done and the efficacy becomes clearer and it is FDA approved, this should change.
We offer payment plans for those in need. Book a consultation to see how we can serve you.
Stem cell therapies that use your own cells (autologous) to stimulate new cell and tissue growth are completely ethical. They also have a lower risk of immune system rejection.
The use of mesenchymal stem cells does not involve embryos or fetuses. These stem cells are harvested and cultured from your own tissue.
This varies by person. Benefits may be seen in a matter of a few months and may continue to stay improved for many years.
The most common side effect is an injection site reaction. There is the possibility, even with your own cells, that there can be immune system reactions to the injected solution.
Most potential serious side effects of stem cell therapy for Parkinson’s disease are theoretical. The concerns raised but which have never actually occurred include a potential risk of tumor formation from stem cells that begin to grow out of control.
It’s possible that your medication needs will change after receiving stem cell treatments, but the effect will be highly individual. We always recommend that our patients work with their doctors to monitor their symptoms and possibly adjust their medications. Please do not change or come off your medications without speaking to your prescribing physician.
In the clinical literature, some Parkinson’s patients have been able to taper off their medications after receiving sufficient stem cell therapy. In a case study, a Parkinson’s patient was able to wean off their medication after 6 months of stem cell therapy treatment. The researchers detected dopamine production from transplanted stem cells as long as 10 years after the treatment.
The only way to know for sure if you are a good candidate is to schedule a consultation and have the doctor assess your health and symptoms. After this, you will be given the options that are best for your individual scenario.
1. Adams, J. D. Possible causes of Parkinson’s disease. Front. Biosci. 26, 387–394 (2021).
2. Da Silva Meirelles, L., Caplan, A. I. & Nardi, N. B. In search of the in vivo identity of mesenchymal stem cells. Stem Cells 26, 2287–2299 (2008).
3. Rustad, K. C. & Gurtner, G. C. Mesenchymal Stem Cells Home to Sites of Injury and Inflammation. Adv. Wound Care 1, 147–152 (2012).
4. Lige, L. & Zengmin, T. Transplantation of Neural Precursor Cells in the Treatment of Parkinson Disease: An Efficacy and Safety Analysis. Turk. Neurosurg. 26, 378–383 (2016).
5. Madrazo, I. et al. Transplantation of Human Neural Progenitor Cells (NPC) into Putamina of Parkinsonian Patients: A Case Series Study, Safety and Efficacy Four Years after Surgery. Cell Transplant. 28, 269–285 (2019).
6. Chang, Y.-H., Wu, K.-C., Harn, H.-J., Lin, S.-Z. & Ding, D.-C. Exosomes and Stem Cells in Degenerative Disease Diagnosis and Therapy. Cell Transplant. 27, 349–363 (2018).
7. McCoy, M. K. et al. Autologous transplants of Adipose-Derived Adult Stromal (ADAS) cells afford dopaminergic neuroprotection in a model of Parkinson’s disease. Exp. Neurol. 210, 14–29 (2008).
8. Mathieu, P., Roca, V., Gamba, C., Del Pozo, A. & Pitossi, F. Neuroprotective effects of human umbilical cord mesenchymal stromal cells in an immunocompetent animal model of Parkinson’s disease. J. Neuroimmunol. 246, 43–50 (2012).
9. Kikuchi, T. et al. Human iPS cell-derived dopaminergic neurons function in a primate Parkinson’s disease model. Nature 548, 592–596 (2017).
10. Mourtzi, T. & Kazanis, I. Endogenous versus exogenous cell replacement for Parkinson’s disease: where are we at and where are we going? Neural Regeneration Res. 17, 2637–2642 (2022).
11. Gordon, J. et al. Sequestration of Inflammation in Parkinson’s Disease via Stem Cell Therapy. Int. J. Mol. Sci. 23, (2022).
12. Stoddard-Bennett, T. & Reijo Pera, R. Treatment of Parkinson’s Disease through Personalized Medicine and Induced Pluripotent Stem Cells. Cells 8, (2019).
13. Gonzalez-Usigli, H. A. Parkinson Disease. Merck Manuals Professional Edition https://www.merckmanuals.com/professional/neurologic-disorders/movement-and-cerebellar-disorders/parkinson-disease.
14. Parkinson’s disease - treatment. nhs.uk https://www.nhs.uk/conditions/parkinsons-disease/treatment/.
15. Sabri, M. A. & Saber-Ayad, M. M. MAO Inhibitors. in StatPearls (StatPearls Publishing, 2022).
16. Gravitz, L. The promise and potential of stem cells in Parkinson’s disease. Nature Publishing Group UK http://dx.doi.org/10.1038/d41586-021-02622-3 (2021) doi:10.1038/d41586-021-02622-3.
17. Stem cell and exosome products. https://www.cdc.gov/hai/outbreaks/stem-cell-products.html (2019).
18. Stoker, T. B. Stem Cell Treatments for Parkinson’s Disease. (Codon Publications, 2018).
19. Piccini, P. et al. Dopamine release from nigral transplants visualized in vivo in a Parkinson’s patient. Nat. Neurosci. 2, 1137–1140 (1999).
Patients Worldwide have been treated at Nashville Regenerative Orthopedics
Are You a Candidate?
Our in-house science team has researched the many types of stem cells available today. Together with our clinical teams, we believe that using your own stem cells are the safest, most effective therapy choice for your body and your health.
Our research-based therapies use your own stem cells to accelerate your healing — without surgery.
Request an Introductory Patient Package
Receive an introductory patient package by email.